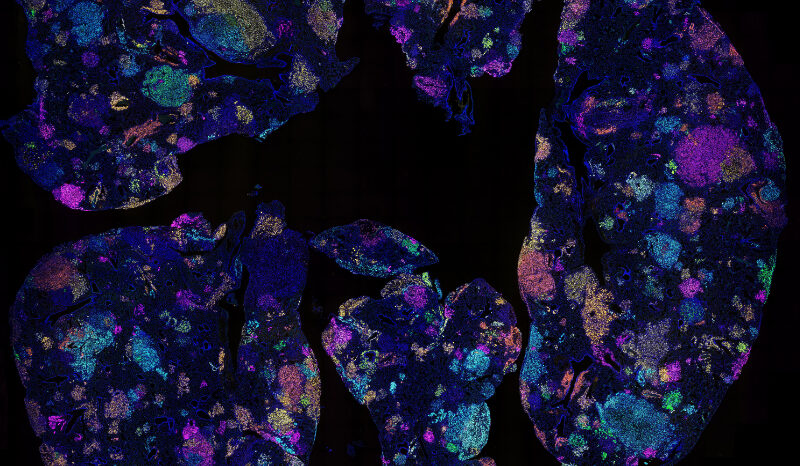
Tuberculosis is caused by infection with the bacterium Mycobacterium tuberculosis. Most commonly, tuberculosis occurs in the lungs.
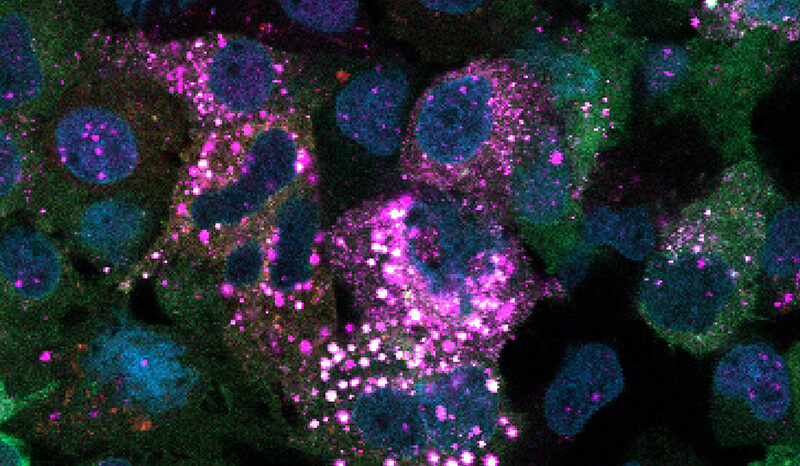
People become infected with M. tuberculosis by inhaling the bacterium. Within the lungs, the bacterium is engulfed by immune cells called macrophages. For other types of bacteria, this will kill the bacteria. However, M. tuberculosis bacteria can survive and reproduce within macrophages.
Tuberculosis-infected macrophages trigger other immune cells to attack them. This leads to inflammation, with a mass of immune cells surrounding the infected macrophages.
In 90 per cent of people infected with M. tuberculosis, the infection becomes ‘dormant’. They do not show any symptoms of the infection, but the infection persists within their body.
In some people, the infection becomes ‘active’. The growth of M. tuberculosis bacteria leads to lung damage. Symptoms of active tuberculosis in the lungs include:
- Cough
- Bleeding into the lungs
- Weight loss
- Fever
When someone has an active tuberculosis infection, they are able to spread bacteria to other people through their respiratory fluids.
Occasionally M. tuberculosis bacteria can spread from the lungs to other parts of the body such as bones or the central nervous system. This can cause a variety of symptoms depending on the site of the infection, such as, for bone tuberculosis, swelling, pain and deformation of joints; or for central nervous system tuberculosis, headaches, confusion and seizures.
It is estimated that 1.8 billion people worldwide are infected with M. tuberculosis. Of these, around 10 million have active illness. Tuberculosis causes 1.5 million deaths each year.