Cohen R, Duval V, Al-Rifai R, Maryam S, Santos-Zas I, Braik R, Diedisheim M, Jouve C, Nicoletti S, Thietart S, Guyon T, Chetrit L, Kral M, Döring Y, Weber C, Loupy A, Domenge O, Livrozet M, Hulot J-S, Sakalli ET, Rizzo G, Saliba A-E, Piollet M, Bruneval P, Tedgui A, Taleb S, Hermine O, Wicks I, Silvestre J-S, Hayat S, Cochain C, Vivier E, Ait-Oufella H. NK cells promote cardiac cell death and regulate myelopoiesis in myocardial infarction. Nature Communications. 2026;:10.1038/s41467-026-71334-x
Swiderski K, Day J, Louis C, Chee A, Trieu J, Vijayakumar P, Crisologo J, Qian H, Gregorevic P, Wicks IP, Lynch GS. FcRn: A novel target to attenuate rheumatoid cachexia in arthritic mice. Biochimica et Biophysica Acta (BBA) – Molecular Basis of Disease. 2026;1872(3):10.1016/j.bbadis.2025.168141
Pires S, Yang W, Frigerio S, Louis C, Scott C, Zhou YL, Cardakli E, Tran N, Hassan-Zahraee M, Ye Z, Hyde C, Hung K, Chen A, Ng C, Grier A, Bank JLC, Lukin D, Scherl E, Targan SR, Diehl GE, Grootjans J, Putoczki TL, Wicks I, Longman RS. Innate lymphoid cells activated by the cytokine TL1A link colitis to emergency granulopoiesis and the recruitment of tumor-promoting neutrophils. Immunity. 2026;59(2):10.1016/j.immuni.2025.12.008
Heydarchi B, D’Silva DB, Wong H, Goddard-Borger ED, Wicks IP. Fc mutagenesis enhances the functionality of anti-RhD monoclonal antibodies. Blood Advances. 2025;9(7):10.1182/bloodadvances.2024015082
Day J, Louis C, Swiderski K, Stock A, Wong H, Yao W, Liu B, Nadesapillai S, Lynch GS, Wicks IP. Periarticular myositis and muscle fibrosis are cytokine dependent complications of inflammatory arthritis. JCI Insight. 2025;10(7):10.1172/jci.insight.179928
Wicks I. Vagus. BioScience. 2024;74(10):10.1093/biosci/biae021
Oxley EP, Kershaw NJ, Louis C, Goodall KJ, Garwood MM, Jee Ho SM, Voo VTF, Park H-Y, Iaria J, Wong LLL, Lebenbaum AG, Wiranata S, Pang ES, Edwards ESJ, D’Silva DB, Hansen J, van Zelm MC, O’Keeffe M, Hogarth PM, Haynes NM, Huntington ND, Wicks IP, Dickins RA. Context-restricted PD-(L)1 checkpoint agonism by CTLA4-Ig therapies inhibits T cell activity. Cell Reports. 2024;43(10):10.1016/j.celrep.2024.114834
Maxwell S, Ross L, Oon S, Wicks IP, Day J. Muscle biopsy practices in the evaluation of idiopathic inflammatory myopathies: An international survey of expert clinicians. Seminars in Arthritis and Rheumatism. 2024;68:10.1016/j.semarthrit.2024.152519
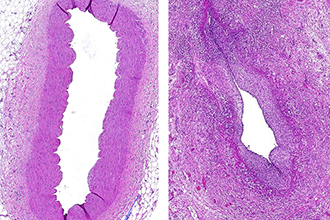
Stock AT, Parsons S, Hansen JA, D’Silva DB, Starkey G, Fayed A, Lim XY, D’Costa R, Gordon CL, Wicks IP. mTOR signalling controls the formation of smooth muscle cell-derived luminal myofibroblasts during vasculitis. EMBO Reports. 2024;25(10):10.1038/s44319-024-00251-1
Chiou S, Al-Ani AH, Pan Y, Patel KM, Kong IY, Whitehead LW, Light A, Young SN, Barrios M, Sargeant C, Rajasekhar P, Zhu L, Hempel A, Lin A, Rickard JA, Hall C, Gangatirkar P, Yip RK, Cawthorne W, Jacobsen AV, Horne CR, Martin KR, Ioannidis LJ, Hansen DS, Day J, Wicks IP, Law C, Ritchie ME, Bowden R, Hildebrand JM, O’Reilly LA, Silke J, Giulino-Roth L, Tsui E, Rogers KL, Hawkins ED, Christensen B, Murphy JM, Samson AL. An immunohistochemical atlas of necroptotic pathway expression. EMBO Molecular Medicine. 2024;16(7):10.1038/s44321-024-00074-6