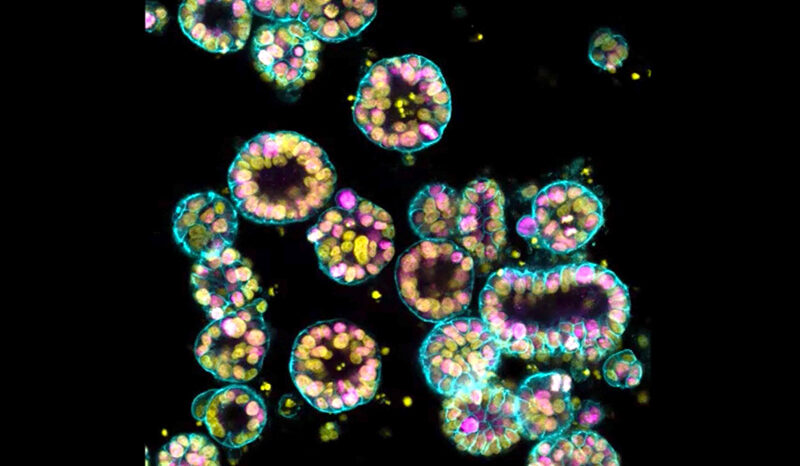
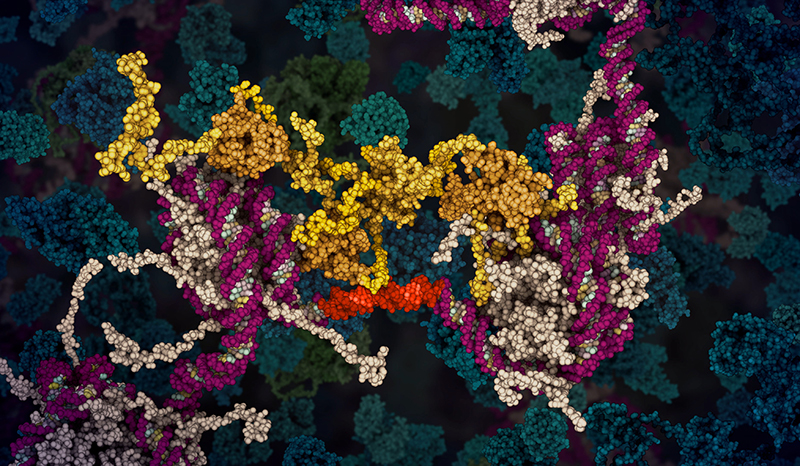
Our lab focus is manipulating cell death for cancer therapy.
My laboratory aims to manipulate the normal cellular pathways to cell death in order to selectively kill cancer cells.
Focusing on a controlled form of cell death called apoptosis, we seek to find genes or proteins that tumour cells depend upon for growth, thus identifying new therapeutic targets that can inform the design of novel anti-cancer drugs.
Our overarching aim is to facilitate the progression of new targeted drugs into the clinic for the treatment of patients with cancer, in particular blood cell derived cancers.