When Professors Geoff Lindeman and Jane Visvader from the institute’s breast cancer research team make a significant discovery it is Avis Macphee who fronts the media to make the news “digestible”.
Macphee also assists with the drafting of patient information and consent documents for clinical trials and research. The fact that applicants for funding for clinical research now have to submit lay summaries and have ordinary people sitting on their research committees testifies to the changes patient advocates like her— “I don’t like the word ‘consumer;’ it implies people have chosen cancer”— helped bring about.
“So I’m the one who will say to Geoff and Jane, ‘ordinary people won’t know what that means.’ Another thing I say is, ‘even if there’s only one person who needs this particular information then it has to be there.”
Exalted and esteemed scientists
Avis Macphee has dined out on the story of how she met husband Alex, a physician, “over a dead body.” They locked eyes about 50 years ago at the Royal Melbourne Hospital (RMH) — Macphee, a medical scientist, worked in morbid anatomy in the 1960s and Alex performed the first post mortem she saw. She also regularly glimpsed Sir Frank Macfarlane Burnet and other esteemed scientists as they headed to the Walter and Eliza Hall Institute two floors up.
But they were exalted,” Macphee recalls. “We were only mere mortals.
Ironic then that Macphee, a breast cancer survivor and patient advocate, found her mission in bridging the divide between the exalted experts and the mere mortals caught in the maelstrom of sickness, fear and hope.
Trialling a cancer treatment in development
In 1992, Macphee, aged 49, and her younger sister had routine mammograms on the same day. The results “threw Freemasons into chaos.” Both women were diagnosed with a tumour in the left breast: her sister’s turned out to be benign, Macphee’s was cancerous, and had spread to 10 out of 14 lymph nodes. She knew her prognosis was grim. The following week she had a modified total mastectomy. Then she was asked to consider participating in a trial at the RMH of three cycles of high-dose chemotherapy, each followed by a “bone marrow rescue” with her own stem cells — the latter, still-experimental treatment enabled by Professor Donald Metcalf’s discovery of the CSF hormone at the institute.
I met Don himself a number of years later at an awards dinner,” Macphee recalls. “He said he never thought he’d be talking to someone who had had the drug.
When the trial was proposed Macphee had a battery of questions for her oncologist.
“Some of those questions are only being answered now. But I talked the language, knew how to research.
“One question I asked was, ‘how do you know that with the bone marrow rescue you’re not re-infusing me with contaminated cancer cells?’ And he said, ‘we don’t.”
She agreed to the treatment – the success of which is self-evident, though it left her with a myopathy of the heart. But she knew the disease was a potential side effect. “I’m probably the only one of the 100 women on that first trial who made a truly informed decision.”
Patient advocacy and support
Shortly thereafter Macphee’s oncologist asked her to speak to a breast cancer patient considering the same radical treatment. She agreed and stayed for three hours; the woman’s young son game to ask Macphee the questions he’d hesitated to ask his mother. It marked the start of Macphee’s extensive CV in patient advocacy, which includes setting up a breast cancer support group at the Bone Marrow Donor Institute, chairing the Health Services Review Council in the mid 1990s and helping establish the Victorian Breast Cancer Research Consortium.
“What women wanted in those early days was support and information— but not just basic stuff. They saw their relationship with clinicians as a partnership. But this wasn’t for everyone. And I really believe that just as every woman has a right to information, if they don’t want information that’s their right too.”
Improvements in survival rates depend on lab breakthroughs
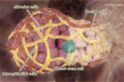
The institute, she notes, was pre-eminent in genetically engineering an entire mammary pad in mice that had been bred to have no mammary tissue. The work, by Dr Mark Shackleton, deepened the understanding of breast tissue development and by extension, cancer formation.
The task is made harder by a “huge backlash” against breast cancer research as critics argue the disease has been attracted disproportionate funding and now “it’s other cancers turn”. Macphee and her fellow activists deny the charge, pointing out that while breast cancer mortality rates are decreasing, thanks to mass screening and improvements in post-surgical therapies, the incidence of the disease is increasing. Major improvements in survival rates now depend on breakthroughs in the lab, but Macphee is troubled by what she sees as inadequate government investment in medical research— the Breast Cancer Consortium shut down for lack of support.
“I don’t think the public understands how dire things are now.”
——-
Vale Avis Macphee
Our dear friend and supporter Avis Macphee passed away on 18 September 2017. She will be missed by her many friends at the institute, and remembered for her inspirational work in patient advocacy.